Limb Trauma
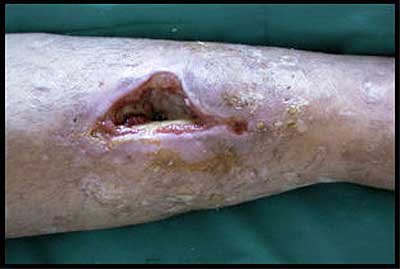
This operation is planned and designed for the reconstruction of the lower limb tegumentary apparatus that, following trauma or demolition in case of tumors or malformations, fails to cover the underlying osteo-muscular structures. Tegumental lesions of the lower limb may also result from vascular damage. A large vessel obstruction caused by a thrombus may lead to ischemia that, even after having healed, leaves behind necrotic tissues that need reconstruction. The same thing happens with crush traumas or when a fracture involves a large caliber artery. Following inferior limb fractures, when bone splinters lacerate the skin, skeletal uncovering complicates any reconstruction. It is indeed frequent to deal with lacerated-contused wounds that can hardly undergo direct closure. The reconstruction should be performed using the simplest surgical procedure, with the least possible failing risks, in order to solve the problem in the shortest time. In fact, the more the osteo-muscular apparatus remains exposed the more likely it is to undergo irreversible damage, both for what concerns organic and functional loss.
A fracture that has synthesized but not yet been covered will cause osteomyelitis with tissue reabsorbtion and stability loss. In other words it is perfectly useless to try to line up the stumps of a long bone if one doesn't provide adequate covering.
Surgical procedure
Direct wound closure is the simplest technique. When tissues are too tight to be sutured one might set up a flap or seal them by means of a dermo-epidermal graft.
Flaps can be cutaneous, fascio-cutaneous or mio-cutaneous, depending on the area that needs reconstruction, on the amount of damage to be repaired and on the peculiar characteristics of the tissues to cover. In fact, while muscles can be covered by means of a simple graft, bones and tendons call for thicker structures. Most of all, the tissues transferred to the defective site need adequate vascularization that can grant revitalization and sufficient antibiotic and anticoagulant supply. To this purpose it is at times necessary to employ anatomical units coming from the couterlateral limb( fascio-cutaneous or cutaneous flaps), that are rotated so as to cover the defect, but maintain a peduncle linked to the donor limb. The connection is kept until enough linkages have created between the flap and the traumatized leg's vital tissues. This technique is called 'Cross-leg'. Alternatively, by means of micro-vascular procedures, one can move mio-cutaneous and muscular flaps to cover heavily damaged areas; a mio-cutaneous unit driven from a site far from the defect is transferred, while the most important vessels are reconstructed.
Scars
As these cannot be classified as aesthetic operations, their cicatricial outcome is not the main concern. Nevertheless it is the plastic surgeon's care to limit residual scarring to a minimum. It is important to avoid the creation of bands and retractions that will limit joint movements. Therefore scars need to be attended in the months following the operation and treated with massages, compressive bandages and hydrating/elasticizing creams.
Operative times
The duration of the procedure can vary. More than one surgical time may be necessary. Plan and sequence of events will be discussed over with the surgeons before the operation.
Anesthesia
During the pre-anesthetization consultation the anesthesiologist evaluates the results of the blood tests and the patient's physical conditions. The operation is performed under spinal or general anesthesia. The kind of anesthesia will be discussed in the presence of both the anesthesiologists and the surgeons before the intervention. Some of the little procedures that serve as preparation or touch-up may be performed under local anesthesia.
Hospital stay
Accordingly to the different procedures, the patient will remain at the hospital until all the dressings are light enough to allow a home-stay (with periodic medical consultations for wound care and bandage changing).
Possible complications
Flaps can show suffering for their reduced blood supply or be contaminated by local infections from the receiving area. A partial tissue necrosis can also occur. Complications, when lesions are wide, may prolong healing time. It is therefore very important to actively collaborate for post-operative care so as to limit possible damages.
